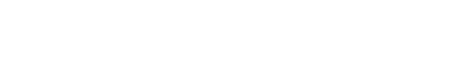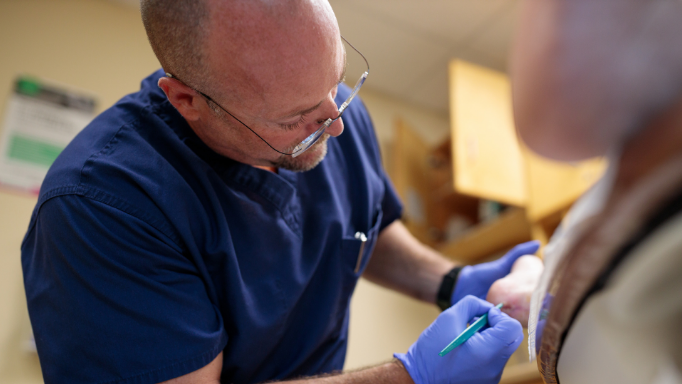
Vermonters are active all four seasons, whether that’s running in the summer, hiking in the fall, or skiing in the winter. Many of us have jobs that keep us on our feet all day as well. So, it’s important to make sure your feet are well-protected. Gifford podiatrist, Dr. Nick Benoit has some tips on how you can stay on your toes when it comes to footcare. He also identifies issues that can happen to the foot.
Dr. Benoit wanted a career in medicine, but he wasn’t quite sure what form that would take. In college, his vision was to be a veterinarian, but after an internship at a vet, decided not to take that path. However, an internship with a podiatrist did make an impact on him.
“He was doing surgery, he was seeing patients in his office and he was helping people with acute issues that needed to be seen,” Dr. Benoit recalls. “The more research I did, I thought it was a good career path.”
Dr. Benoit attended podiatry school in Des Moines, Iowa and completed his surgical residency in Binghamton, NY, before getting a job offer at Gifford in 2007.
“I was blown away,” Dr. Benoit said. “Walking in the doors the first time I said, I think I’m going to retire from this place. I’ve been here ever since. I love it here.”
In a normal week, Gifford’s three-person podiatry team sees patients in Randolph, Sharon and Berlin as well as the inpatient consultations and calls from Gifford’s Emergency Department.
“We work really hard to get people into our clinic in a timely fashion,” Dr. Benoit said. “Every problem that an individual has is important to them and we try to make it our priority to see them as quickly as possible.”
Thursday is Dr. Benoit’s surgery day.
“It’s the day where you’re able to execute the skills you were trained to do,” Dr. Benoit said.
Not every foot and ankle problem needs surgery. In fact, many issues can be solved with appropriate education and conservative management.
“If it is a real concern, we’re happy to see you,” Dr. Benoit said. “Even if it’s nothing, it gives you peace of mind. It’s better to have it looked at than wait until something goes really bad.”
If you do call Gifford with foot or ankle pain, our nursing and support staff are trained to evaluate patients with simple questions and they’ll know if someone needs to be seen right away.
According to Dr. Benoit, if your foot is swollen, red, feels hot, or you can’t walk on it, “that’s a big deal.” If it’s mildly achy, inconsistent discomfort, and it’s not significantly hampering your physical activities, Dr. Benoit says you could wait a while to see if it goes away.
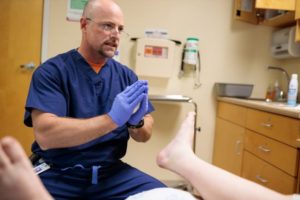 Here are some thoughts Dr. Benoit has on common foot and ankle issues he sees regularly:
Here are some thoughts Dr. Benoit has on common foot and ankle issues he sees regularly:
Stress Fractures
“I see a fair amount of stress fractures. A lot of them are Emergency Department or primary care referrals for pain that is persistent for weeks or months, often resulting in swelling. Stress fractures are often caused by overuse of the foot. If you’re on the couch all winter then decide to run five miles one day in the spring, you’re increasing your chances of getting one. However, getting a stress fracture can be a result of just bad luck. Shoe gear can also play into it or they can also be a result of vitamin D deficiencies. Stress fractures may not be seen on an x-ray if you go to primary or urgent care. For treatment, I’d suggest backing off of activities for the time being.”
Flatfoot
“Flatfooted folks don’t always have issues. I’m not concerned with people having too high of an arch or no arch at all. It’s more about being concerned if they have pain.”
Numbness or Tingling
“It can be from a result of chronic back pain, entrapment of a nerve, footwear, or just from a certain activity. Normally it’s not a circulatory issue.”
Ingrown Toenails
“These hurt. The nail irritating the skin creates a portal of entry for bacteria. Unless the offending portion of the nail is removed, it’s not going to go away. Ingrown toenails can result from cutting a nail the wrong way, fungus in the toenail, or it’s jammed in a shoe wrong and it keeps getting pushed against the edge. To permanently fix the issue, I would consider a simple nail cutting procedure to remove all or a portion of the nail.”
Plantar Fasciitis and Bone Spurs
“Plantar Fasciitis is inflammation of a band of ligaments on the bottom of the heal. People often think they have bone spurs in the heel when 90% of the time it’s Plantar Fasciitis. You need good supportive shoes to prevent this. Walking around your house barefoot isn’t good for this either. Of course, stretching is the mainstay treatment for preventative care. Everyone needs to stretch more, especially as we get older. If you have a twinge of pain by the heel, re-evaluate what you’re doing and the type of shoes you’re wearing. Rarely is surgery needed and it can be managed with education, stretching, inserts, and anti-inflammatories. If you do have a bone spur, surgery is the common form of treatment.”
Ankle Sprains and Breaks
“We see a lot of ankle sprains and many of them are referrals from our Emergency Department. The thing about ankle sprains, is you need to aggressively treat them. With aggressive treatment, I find people get better faster and over the long haul, the ankle is better. We want to immobilize the ankle, get the swelling under control, stabilize it and eventually see a physical therapist. If we can get that ankle actively moving again, your outcomes are going to be better over time.”
Gifford’s Podiatry team also offers complete foot and ankle evaluations to determine if there are any areas of concern in a diabetic patient. Foot problems are common in people with diabetes. They can happen over time when high blood sugar damages the nerves and blood vessels in the feet. The nerve damage, called diabetic neuropathy, can cause numbness, tingling, pain, or a loss of feeling in your feet. High-risk patients who have a history of peripheral neuropathy, PVD, history of ulceration, or history of amputation are of particular concern.
“Part of my job oftentimes is amputating feet or parts of the feet that could have been resolved with simple measures. If we can prevent a problem from occurring, then I wouldn’t have to be aggressive on your foot or ankle. If your blood sugars are in check and you don’t feel any issues with your feet, then typically I’d see a person with diabetes about once a year.”
Finally, we asked Dr. Benoit about proper footwear and insoles.
“Obviously if you’re going hiking, you should wear good, lace-up hiking boots. You don’t need custom orthotics, just proper footwear for the activity and the environment in which you’re doing it. First, evaluate your footwear. If your footwear is well over a year and a half old and you put a lot of miles on them, start with some new shoes. Not everyone needs insoles. Your insoles are only going to be as good as the shoes you put them in. Custom orthotics should work better than over-the-counter products and last longer. Having a dedicated pair of sneakers or shoes is a good idea. You have different clothes for work and certain outdoor or indoor activities, you should have the same philosophy for your footwear.”
Many of Gifford’s podiatry patients work hard or play hard outdoors and they need to get back to work. Dr. Benoit says it’s the responsibility of the podiatry team to find treatment plans that, “suit the individuals around us.”
“I couldn’t imagine my feet hurting bad enough that it keeps me doing something that I want to do. We like to educate people by talking to them and answering their questions.”
For more information on Gifford’s Foot Care Services, go to: https://giffordhealthcare.org/service/podiatry/